
Journal of the Bahrain Medical Society
Year 2018, Volume 30, Issue 2, Pages 6-9
https://doi.org/10.26715/jbms.2_12a082018Wael Mohamed Tahseen1*, Hani Ebrahim Ahmed AlFadel1
1Radiologist, Department of Radiology, Bahrain Defense Force Hospital, Riffa, Bahrain
*Corresponding author:
Wael Mohamed Tahseen, Radiologist, Department of Radiology, Bahrain Defense Force Hospital, Riffa, Bahrain, Tel.:0097335386056, Email: wael.tahseen.bdf@gmail.com
Received date: July 09, 2018; Accepted date: August 12, 2018; Published date: September 04, 2018

A 67-year-old Bahraini male patient, diabetic and hypertensive, presented to the Emergency department with complaints of 3-days history of shortness of breath, abdominal distension, and constipation without abdominal pain. Clinical evaluation and laboratory investigations revealed lower abdominal tenderness and rebound tenderness as well as status of septic shock. Contrast enhanced computed tomography revealed inflamed vermiform appendix with pneumoretroperitoneum and abdominal wall emphysema associated with abdominal wall edema. Surgical laparotomy was performed which revealed retroperitoneal perforation of the appendix associated with pus and air in the retroperitoneum and the abdominal wall. Appendectomy was performed along with drainage of retroperitoneal as well as abdominal wall pus. The case represents an uncommon complication of acute vermiform appendix inflammation with retroperitoneal perforation into the abdominal wall. This case indicates that a possibility of intra-abdominal pathology should be raised in patients with subcutaneous surgical emphysema of the chest and abdomen.
Keywords: Acute appendicitis, atypical, computed tomography, subcutaneous emphysema, retroperitoneal
Acute inflammation of the vermiform appendix is a commonly encountered disease with an approximate lifetime incidence of 7%. The gender distribution is about 8.6% and 6.7% among males and females, respectively; with higher incidence in patients aged 15–19 years (males) and 10–14 years (females). Perforation is observed in 20–30% of cases, which increases the frequency of complications, such as wound infection, abscess formation, and peritonitis.1,2
On an international scale, the incidence of acute appendicitis is increasing in newly industrialized countries to the degree that it overwhelms the incidence in the western countries. There is dearth of data regarding the incidence of acute appendicitis in developing countries.3
Acute appendicitis is a multifactorial disease and epidemiological comparisons between developed and developing countries indicate an association with the degree of societal economic development.3 Acute appendicitis, occasionally, is associated with high morbidity and mortality yet difficult to diagnose, however, on-time evaluation can prevent it. The atypical presentation of appendicitis is rare and requires high suspicion.4
A 67-year-old man with a history of type 2 diabetes mellitus and hypertension presented to the Emergency department in our hospital. The patient had a 3-day history of shortness of breath, abdominal distension, and constipation without abdominal pain and blood per rectum.
On admission, the patient was diagnosed for septic shock; the vitals were recorded: blood pressure 100/42 mmHg, pulse rate 42 beats/min, and respiratory rate 35 beats/min. Leukocytosis and elevated C-reactive protein and lactate along with acute renal impairment were documented. Ventricular tachycardia was detected and required shock cardio version was administered. Abdominal examination revealed distension and lower abdominal tenderness along with guarding and rebound; sluggish bowel movements were noted as well.
Contrast enhanced Computed tomography (CECT) performed in dual phases of contrast enhancement with nonionic iodine based intravenous contrast and arterial bolus tracking technique. Using In the arterial phase, 120 kV and 304 mA was used, whereas, in the venous phase 140 kV and 200 mA was used. Two slices with thickness of 2 mm and 3 mm were used for the arterial and venous phase, respectively. CECT revealed abdominal wall emphysema (Figure 1) and right iliac fossa inflammatory changes around the caecum manifested as para-colic fat stranding and thickened hyper enhanced appendix wall with increased cross-sectional diameter reaching 14.5 mm (Figure 2). Associated extensive pneumoretroperitoneum and abdominal wall inflammatory edema (figure 3) was detected; however, no evidence of penumoperitoneum.
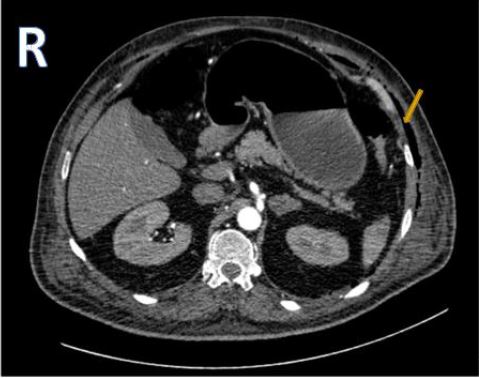
Figure 1: Axial contrast enhanced computed tomography scans of the abdomen showing abdominal wall emphysema on the left side (yellow arrow)
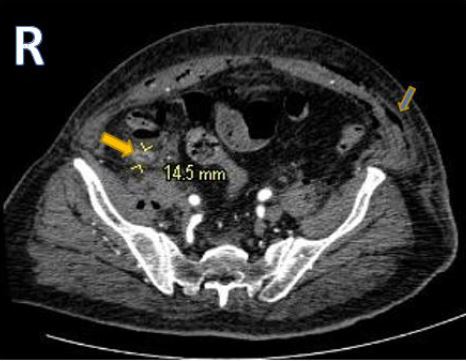
Figure 2: Axial contrastenhanced computed tomography scans of the abdomen showing hyper enhanced thickwall of distended vermiform appendix with surrounding fat plans stranding(yellow arrow) and associated abdominal wall emphysema (blue arrow)
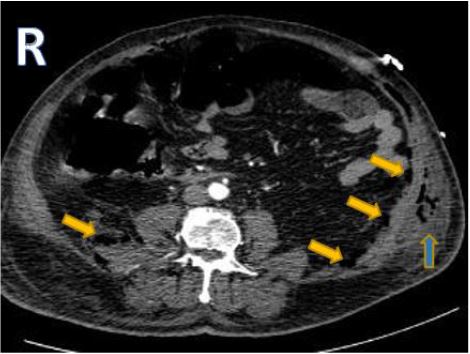
Figure 3: Axial contrast enhanced computed tomography scans of the abdomen showing abdominal wall emphysema and inflammatory edema notably on the left side (blue arrow) and retropneumoperitoneum (yellow arrows)
The patient underwent laparotomy with midline incision, dissection in layers below peritoneum, peritoneal cavity and exploration with mobilization of caecum and ascending colon. Foul smelling retro peritoneal pus and perforated appendix with free faecolith were detected; free pus in the anterior abdominal wall was drained after exploration. Appendectomy was performed with purse string suture and retroperitoneal drainage of pus was performed with insertion of a drainage catheter. The abdominal wall was then closed with polydioxanone sutures followed by skin-clip closure of the skin.
Post-operative diagnosis revealed perforated appendicitis with leaked bowel air and content to the retroperitoneal space causing a consequential retroperitoneal and soft tissue infection of the abdominal wall.
Pathological assessment of the resected appendix specimen revealed gross pathological changes, including congested and perforated appendix. Histopathological assessment showed mucosal ulceration and heavy transmural acute inflammatory cell infiltrate with perforation.
Postoperatively, the patient was admitted to the intensive care unit. On postoperative day four, the patient became hemodynamically unstable, blood pressure dropped to 60/28 mmHg and heart rate reduced to 40 beats/min, followed by reduced heart rate leading to asystole. Cardiopulmonary resuscitation was performed; however, the patient demised.
Globally, acute appendicitis is the most common abdominal emergency. The risk probability of appendicitis during life is approximately 7%.5 Early management is essential to prevent morbidity and mortality. Typically, patients initially suffer from vague abdominal pain, which later shifts to the right lower quadrant. In the elderly and pediatric patients, however, an atypical presentation is observed, which can result in delayed and/or inappropriate diagnosis resulting in life-threatening complications.6
Review of literature revealed that diverticulitis, perforated acute appendicitis, colorectal malignancy, Crohn’s disease, abdominal trauma, and rarely, suppurative iliac lymphadenitis, pyelonephritis, and abdominal tuberculosis cause retroperitoneal abscess formation. The inflammatory process could spread through abdominal wall, thigh, groin, psoas muscle and perinephric space, but few literatures discussed perforated retro-caecal appendicitis with widespread subcutaneous air of abdominal wall.5,7–9
Ishigami et al. reported various complications of acute appendicitis, including necrotizing infections of the abdominal wall or the lower limb; one case reported infection of the perineum and the external genitalia.10
The complicated acute vermiform appendix inflammation represents a retroperitoneal air, which has escaped to the subcutaneous space of the abdominal wall. Due to its location, a perforated acute appendicitis in the retroperitoneal area can result in atypical manifestations. Infection and air can extend through connected compartments either through anatomical connections or pathological connections by perforation through anatomical boundaries, leading to emphysema and infection in unusual locations. Due to the retroperitoneal location of infection in our patient, regular peritoneal manifestations of appendicitis were absent. Multiple routes are present through which the intra-abdominal infection could reach the unusual locations. Infection can spread deep to the inguinal ligament to reach the psoas and femoral sheath as well as the femoral canal through the sacro-sciatic notch and obturator canal. Further, it spreads from the abdominal wall to the subcutaneous tissue through the lumbar triangles or directly by penetration of the pelvic floor. Fulminant course with generalized cellulitis and septicemia can occur.10–12 The appendix in a retro-caecal position is frequently reteoperitoneal in location.13
Delayed presentation is the leading cause of morbidity and mortality. Early presentation and diagnosis, use of appropriate antibiotics, and surgical intervention are important in reducing the morbidity. We are, hence, reporting a rare case. Computed tomography scans of abdomen and pelvis is the gold standard imaging modality, which accurately define the anatomical location of inflammation and the concurrent intra-abdominal pathology. Early presentation can guide the clinician to a precise diagnosis and extension of the involvement of the retro peritoneum and the subcutaneous tissue.14,15
Even though perforated appendicitis, as an etiology of a rapidly progressive soft tissue infection of the abdominal wall is very rare, it should be considered in the differential diagnosis of abdominal wall cellulitis. Contrast enhanced computed tomography aids in the assessment of the elderly patients with constellation of manifestations out of proportion of the presenting abdominal clinical presentation.